Appendicitis is an inflammation of the appendix, a finger shaped pouch that projects from your colon on the lower right side of your abdomen.
The Causes of Appendicitis —
- Appendicitis happens when the appendix gets blocked, often by poop, a foreign body, or cancer.
- A blockage in the lining of the appendix that results in infection is the likely cause of appendicitis. The bacteria multiply rapidly, causing the appendix to become inflamed, swollen and filled with pus. If not treated promptly, the appendix can rupture.
The Symptoms of Appendicitis —
Signs and symptoms of appendicitis may include:
- Sudden pain that begins on the right side of the lower abdomen
- Sudden pain that begins around your navel and often shifts to your lower right abdomen
- Nausea and vomiting soon after belly pain begins
- Pain that worsens if you cough, walk or make other jarring movements
- Swollen belly
- Low-grade fever that may worsen as the illness progresses
- Constipation or diarrhea
- Abdominal bloating
- Flatulence
The site of your pain may vary, depending on your age and the position of your appendix. When you’re pregnant, the pain may seem to come from your upper abdomen because your appendix is higher during pregnancy.
Three signs will be positive here —
- Rovsing’s sign — It is a sign of appendicitis. If palpation of the left lower quadrant of a person’s abdomen increases the pain felt in the right lower quadrant, the patient is said to have a positive Rovsing’s sign.
- Psoas Sign — It is a medical sign that indicates irritation to the iliopsoas group of hip reflexors in the abdomen, and consequently indicates that the inflamed appendix is retrocaecal in orientation (as the iliopsoas muscle is retroperitoneal)
- Obturator sign — The Obturator sign or Cope’s obturator test is an indicator of irritation to the obturator internus muscle.
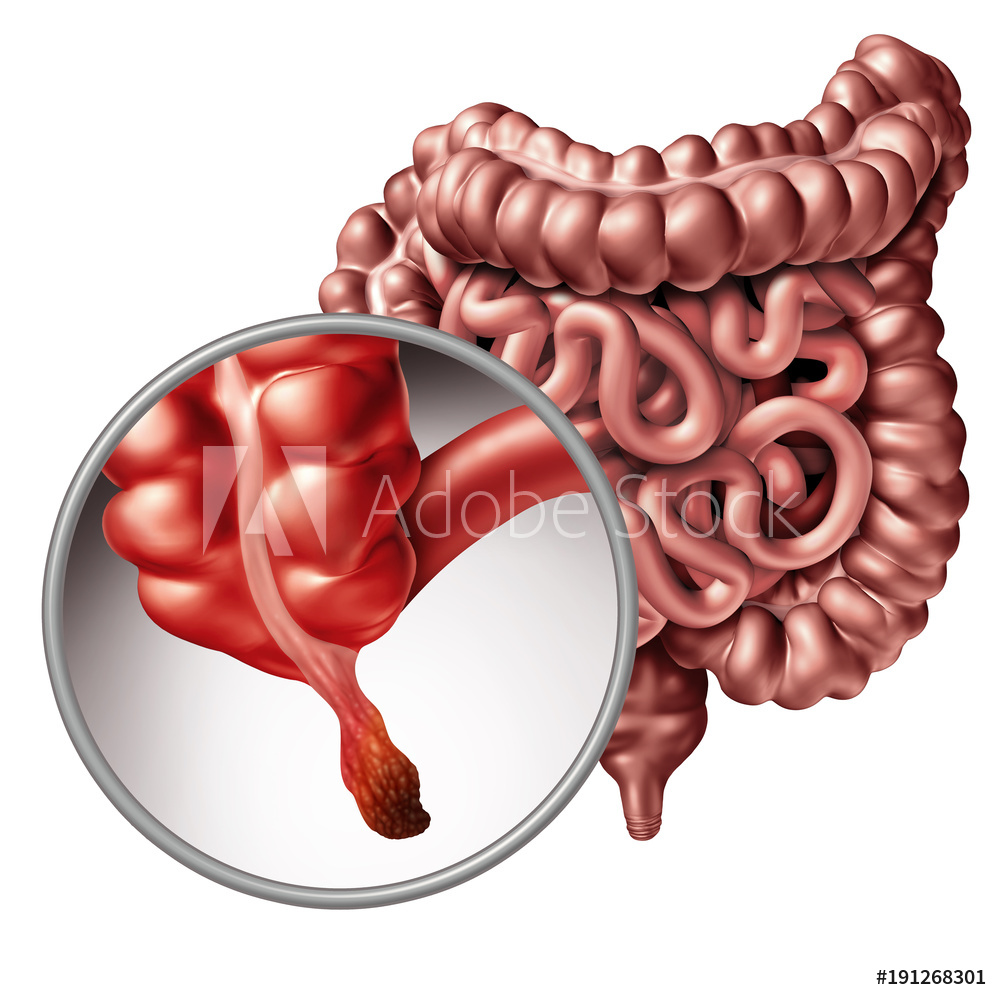
The Complications of Appendicitis —
Appendicitis can cause serious complications, such as:
- A ruptured appendix. A rupture spreads infection throughout your abdomen (peritonitis). Possibly life-threatening, this condition requires immediate surgery to remove the appendix and clean your abdominal cavity.
- A pocket of pus that forms in the abdomen. If your appendix bursts, you may develop a pocket of infection (abscess). In most cases, a surgeon drains the abscess by placing a tube through your abdominal wall into the abscess. The tube is left in place for about two weeks, and you’re given antibiotics to clear the infection.
Once the infection is clear, you’ll have surgery to remove the appendix.
Diagnosis of Appendicitis —
To help diagnose appendicitis, your doctor will likely take a history of your signs and symptoms and examine your abdomen.
Tests and procedures used to diagnose appendicitis include:
- Physical exam to assess your pain. Your doctor may apply gentle pressure on the painful area. When the pressure is suddenly released, appendicitis pain will often feel worse, signaling that the adjacent peritoneum is inflamed.
Your doctor may also look for abdominal rigidity and a tendency for you to stiffen your abdominal muscles in response to pressure over the inflamed appendix (guarding).

- Blood test — This allows your doctor to check for a high white blood cell count, which may indicate an infection.
- Urine test — Your doctor may want you to have a urinalysis to make sure that a urinary tract infection or a kidney stone isn’t causing your pain.
- Imaging tests — Your doctor may also recommend an abdominal X-ray, an abdominal ultrasound, computerized tomography (CT) scan or magnetic resonance imaging (MRI) to help confirm appendicitis or find other causes for your pain.
Treatment of Appendicitis —
Appendicitis treatment usually involves surgery to remove the inflamed appendix. Before surgery they give a dose of antibiotics to treat infection.
- Surgery to remove the appendix — Appendectomy
- Draining an abscess before appendix surgery — If your appendix has burst and an abscess has formed around it, the abscess may be drained by placing a tube through your skin into the abscess. Appendectomy can be performed several weeks later after controlling the infection.
Lifestyle to be followed —
Expect a few weeks of recovery from an appendectomy, or longer if your appendix burst.
To help your body heal:
- Avoid strenuous activity at first. If your appendectomy was done laparoscopically, limit your activity for three to five days. If you had an open appendectomy, limit your activity for 10 to 14 days.
- Support your abdomen when you cough. Place a pillow over your abdomen and apply pressure before you cough, laugh or move to help reduce pain.
- Get up and move when you’re ready. Start slowly and increase your activity as you feel up to it. Start with short walks.
- Sleep when tired. As your body heals, you may find that you feel sleepier than usual. Take it easy and rest when you need to.
Ayurveda Treatment Principle —
- Antarvidradhi and Dhatu pakahara oushadhas.
- Aama pachana oushadhas
- Chronic conditions can be considered as Antharvidradhi and should be treated with Aamapachanam and Antarvidradhi chikitsa is employed.
Kashayam —
- Amrtotaram Kashayam — 60 ml morning and night before food.
- Trayanthadi Kashayam — 60 ml morning and night before food.
- Kaidaryaadi Kashayam — 60 ml morning and night before food.
Churnam —
- Kaidaryadi churnam 1 tsp along with buttermilk morning and night after food.
Gulika —
- Vivadi Gulika
- Dhanvantara Gulika
- Sudarshana Gulika
- Vettumaran Gulika
- Sanjivani Vati
Ghritam — (Recovery phase)
- Grahanyantaka Ghritam
- Changeryaathi ghritam
- Trayantyadi ghritam
- Varanadi Ghritam
Aasavam —
- Madhukasavam
- Sudarshanasavam
- Parpatakarishtam
- Amritarishtam
Rasa Oushadhas —
- Agni kumara rasa
- Abhraka Bhasma
- Sangu Bhasma
- Svarnamakshika Bhasma
Hello!!
I’m Dr. Malini Bhat MD (Ayu); an Ayurvedic Doctor and a health blogger. Follow me on social media to get daily health tips which you can easily adapt to a healthy lifestyle.